Its proactive development of a sepsis care bundle predated the introduction of national policies and guidelines to improve sepsis outcomes – but the real-world demands on its clinical staff created a margin for human error in its delivery. The trust’s performance against national quality improvement indicators was falling short.
The subsequent deployment of mobile technology to help expedite diagnosis and escalate treatment pathways has transformed sepsis care across the integrated organisation. County Durham & Darlington is now among the best performing trusts in England in its identification and treatment of patients with sepsis.
This is their story.
The national challenge: improving sepsis outcomes
Improving outcomes for patients with sepsis is a major NHS priority. The condition, which annually costs the NHS an estimated £2.5 billion, claims at least 44,000 lives in the UK each year. Around 14,000 of these deaths are preventable. Studies suggest that patients diagnosed and treated within one hour of presenting with sepsis have an 80% survival rate. However, mortality rates increase significantly with every subsequent hour that treatment is delayed; after the sixth hour, a patient has only a 30% survival rate. A 2015 report by the National Confidential Enquiry into Patient Outcome and Death found that in many cases, sepsis diagnosis was delayed because HCPs failed to record and respond to basic vital signs. The National Early Warning Score (NEWS) has shown to be a reliable indicator of patients at risk of deterioration. It is widely accepted that a NEWS of >5 should always prompt a screen for sepsis.
Measures to improve the early recognition and treatment of sepsis have increased in recent years. In 2013, a report by the Health Service Ombudsman for England identified clear failings in how NHS trusts were managing the crucial first few hours of patients presenting with sepsis. It urged wholesale action to address shortcomings and eliminate preventable deaths. In December 2015, NHS England published its first sepsis plan, a cross-system action plan to increase awareness of sepsis and support early identification and prompt treatment. The plan, which followed the introduction of CQUIN goals for sepsis in March 2015, was reinforced by a NICE Clinical Guideline for sepsis the following year. In November 2016, the CQUIN indicators for sepsis and antimicrobial resistance were combined into a single indicator focused on reducing the impact of serious infection. NHS England issued its second sepsis action plan in September 2017. The updated strategy coincided with publication of a NICE Quality Standard for sepsis first recommended in the inaugural plan.
In each case, policies and guidelines focus on the importance of early recognition of sepsis followed by timely antibiotic treatment, with quality improvement measurements recommending patients receive a broad-based IV antibiotic within one hour of presenting symptoms of sepsis.
Despite the measures, sepsis remains a challenge for many trusts across the NHS in England. Performance against national quality indicators remains variable. Analysis of NHS data broadcast recently by the BBC indicated that 37% of patients that need antibiotics for sepsis are not receiving them within the recommended time, while 14 trusts are only screening one in every two people with signs of sepsis. UK Health Secretary, Jeremy Hunt, has conceded that although the picture is much improved from two years ago, preventable deaths from sepsis are still happening. There remains much to do.
A regional challenge: County Durham & Darlington NHS Foundation Trust
County Durham & Darlington NHS Foundation Trust is one of the UK’s largest integrated healthcare organisations, providing acute and community services to over 650,000 people in the North East of England. In the past three years, the organisation has worked hard to strengthen its infrastructure and processes to improve patient safety across all of its hospital sites, including an improvement in sepsis outcomes across its two acute sites; Darlington Memorial Hospital and University Hospital of North Durham.
Although County Durham & Darlington had no discernible problem with sepsis-related deaths, its focus on sepsis intensified in 2014 when reducing sepsis mortality was identified as a regional priority in the North East. In October 2014, the trust’s 2015-17 clinical quality and safety improvement strategy set out a blueprint to support the early identification and treatment of sepsis. The plan included the trust-wide roll-out of a sepsis care bundle – built around the core principles of the Sepsis Six – and the development of an audit tool to identify outcome measures. However, despite the approach enjoying good clinical buy-in, early results were disappointing. High demand on wards meant that compliance among clinical teams was suboptimal, with nursing teams occasionally – understandably – forgetting to screen patients for sepsis. In 2015/16, the number of sepsis patients receiving antibiotics within the one-hour timeframe was low.
Lisa Ward, Lead Nurse responsible for sepsis at County Durham & Darlington, says: “The nurses in our clinical areas do not deliberately forget to screen for sepsis – they do so because they’re exceptionally busy looking after patients. We knew that if we were to improve our compliance and increase the early diagnosis and treatment of patients with sepsis, we needed to give our clinical teams greater support in remembering the key components of the care bundle. We recognised that technology gave us the best chance of providing that support.”
In 2016, the organisation adopted a new regional infection screening tool that had been developed collaboratively with other trusts in the North East. However, in line with the trust’s strategy to support its staff with streamlined processes and systems that maximise the use of technology, County Durham & Darlington chose to deploy the new tool electronically, building on existing capability within the trust. “We didn’t want to launch it on paper and implement yet another change for people to remember,” says Lisa Ward. “We wanted to make it part of our existing electronic system – Nervecentre. Our performance is now so much better.”
The solution: a mobile platform
In November 2016, County Durham & Darlington, in alignment with its Health Informatics strategy, took steps to extend its use of Nervecentre to support sepsis screening and the associated escalation of care. “This was a natural development,” says Paul Latimer, Lead Nurse, Special Projects. “Nervecentre already supports other elements of our organisation, not least with electronic observations recording and escalation. Observations are the foundation of clinical decision-making. Certainly, they’re the first port of call when screening for sepsis – generating an early warning score (EWS) that’s a key determinant in the identification process. Crucially, Nervecentre uses mobile technology – giving our teams real-time access to vital information wherever they are in the hospital via hand-held, mobile devices. The ability to get the right information to the right person at the right time helps minimise risk, reduce human error and, most important of all, accelerate timely care. This is proving invaluable in our attempts to improve sepsis outcomes.”
The Nervecentre platform uses vital signs, EWS and pathology results to inform the early diagnosis of sepsis. Algorithms, based on sepsis indicators and NICE guidance, are applied to local/regional clinical rules to help identify early onset. Critically, when a patient presents early indications of sepsis, the platform’s intelligent alert system immediately alerts the right clinicians and nurses to ensure that care is appropriately escalated, prioritised and carried out. Moreover, the system not only alerts clinical staff, it intuitively links with pathology to provide clear visibility of when results have been received or are still to be reviewed. The combination of the algorithm, automated escalation and task prioritisation helps eliminate the human factors that can delay the identification and treatment of sepsis.
County Durham & Darlington’s deployment of the sepsis application was piloted in April 2017 before being rolled-out fully across its acute sites the following month. It has transformed operational processes across the trust and driven substantial improvements in the care of adult patients with sepsis. “Fundamentally, the organisation has a greater understanding and visibility of its sepsis population,” says Paul Latimer. “Prior to the deployment, the trust could neither quantify nor prove the size of its sepsis problem at any given time, presenting an immediate barrier to attempts to drive quality improvement. Moreover, our clinical staff are empowered by having real-time information – in their pockets, wherever they are – that helps them prioritise and respond to patient needs quickly and appropriately. This rules out human error and drives up quality.”
The outcomes
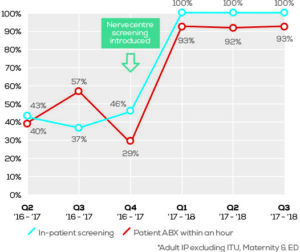
The deployment of the sepsis application, underpinned and powered by the bedrock of Nervecentre’s e-Observations, has meant that every single adult in-patient admitted to County Durham & Darlington’s acute hospitals is now screened for sepsis. This represents a significant improvement on previous performance. Prior to the introduction of Nervecentre screening, 46% of in-patients were screened for sepsis – with levels as low as 37% in Q3 2016/17. By May 2017, this had climbed to 100%.
Similarly, the number of adult patients with sepsis receiving antibiotic treatment within one hour of diagnosis has risen significantly. The methodology used to record data in 2016/17 is different from that deployed in 2017/18 – improvements in the identification of sepsis means that the data sample now includes a higher proportion of patients with the condition. Despite this important nuance, the comparative outcomes are impressive. Prior to the introduction of Nervecentre screening, the number of patients administered antibiotics within one hour of a sepsis diagnosis was 29%. In May 2017, that figured had grown to 93% – and has continued to perform in excess of 90% in the months that have followed.
Paul Latimer says: “Our goal has always been to provide assurance to patients that County Durham & Darlington NHS Foundation Trust is a safe environment that delivers high quality care. Our work with Nervecentre is a great example of that commitment. The mobile platform is helping us support our staff with tools to recognise – and respond to – a potentially life-threatening condition. And it’s allowing us to provide the assurance that every patient that comes into our care will be screened for sepsis – and treated promptly and appropriately.”
Conclusions
County Durham & Darlington NHS Foundation Trust’s 2017-2020 quality improvement strategy reinforces an organisational vision that sets out to be “Right First Time, Every Time.” Technology will play a key role in achieving that vision – but its adoption is an incremental journey. The trust’s use of Nervecentre is making an important contribution to patient care and evolving in response to emergent challenges.
Andrew Jennings, Clinical Chief Information Officer (CCIO) at County Durham & Darlington says: “The whole of the Patient flow management and e-Observations system in general has transformed the way we work. It has given our clinical teams, and in particular our nursing staff, the information and tools to monitor and therefore treat patients more effectively. We’ve subsequently been able to build on that information – and connect it with other systems such as pathology – to inform how we intelligently respond to the growing challenge of sepsis. Nervecentre has changed how we do things, without being a burden on our teams. Effective technology is liberating – it not only provides real-time information, it gives us back the time to do something with it to drive up healthcare quality.
“The introduction of Nervecentre has been hugely positive. It’s been used – and continues to be used – to inform processes, accelerate care and help us to deliver safe, effective high quality healthcare. This has certainly proved the case in our identification and treatment of patients with sepsis.”