SUCCEEDING IN SEPSIS:
The timely identification of conditions such as sepsis and AKI, and the early initiation of treatment, are essential for delivering good patient outcomes. While hospitals hold well established protocols for these conditions, those protocols can be complex – involving multiple members of the patient’s care team, and multiple decision points. The complexity increases the potential for human error, delays and miscommunication – all of which can adversely impact patient safety.
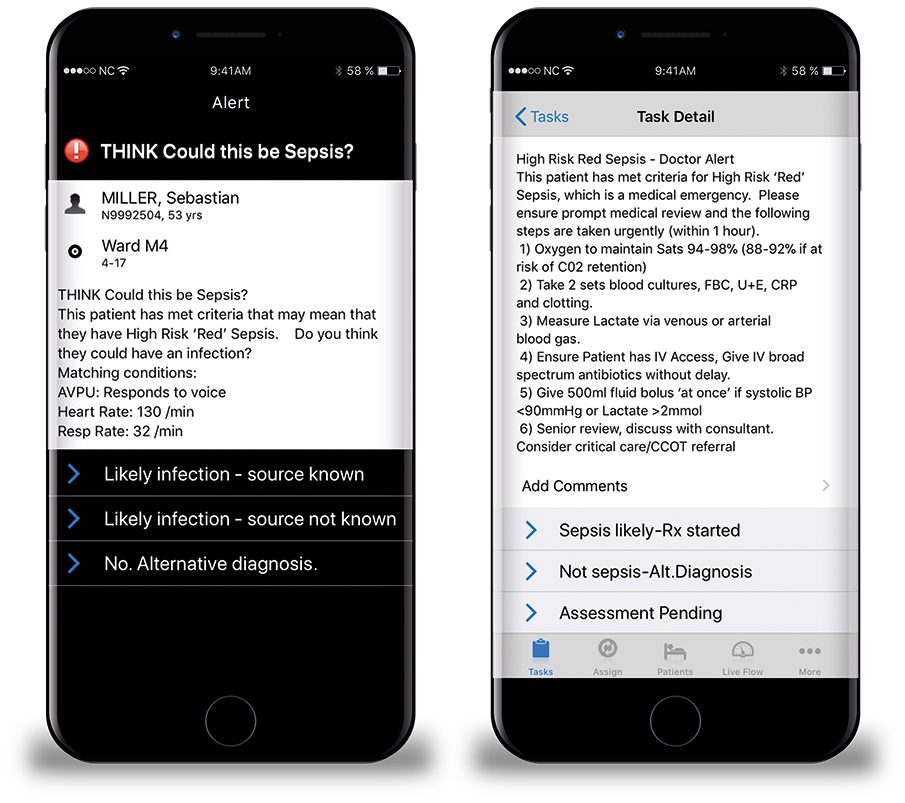
Nervecentre clinical rules enable the automation of time-critical workflows, such as screening of sepsis and commencement of the sepsis 6 bundle, by constantly reviewing data received from multiple information sources, and using escalations and realtime alerts to reduce the delay between steps in the screening and treatment process.
Nervecentre Mobile ‘clinical rules’ instantly identifies sepsis markers and incorporates the NEWS2 scoring system. The individual parameters outlined in the NICE guidelines such as heart rate >130 are programmed as ‘conditions’ and then the rules assess one or a combination of these ‘conditions’ to trigger workflow. Positive triggers allow handover notes, patient tags and tasks sent to the correct clinicians to ensure timely identification and treatment of patients with suspected sepsis.
County Durham & Darlington NHS Foundation Trust is one of the UK’s largest integrated healthcare organisations, providing acute and community services to over 650,000 people in the North East of England. In the past three years, the organisation has worked hard to strengthen its infrastructure and processes to improve patient safety across all of its hospital sites, including an improvement in sepsis outcomes.
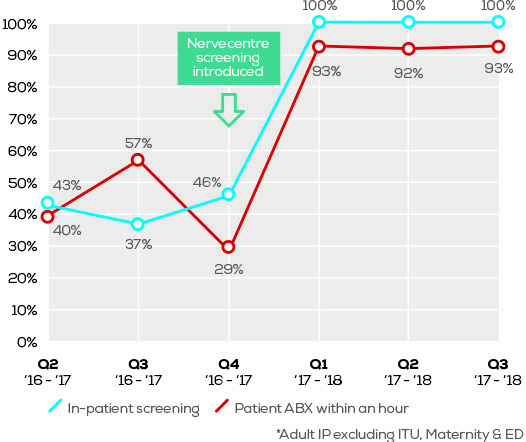
Prior to the introduction of Nervecentre screening, 46% of in-patients were screened for sepsis – with levels as low as 37% in Q3 2016/17. By May 2017, this had climbed to 100%*.
Similarly, the number of patients with sepsis receiving antibiotic treatment within one hour of diagnosis has risen significantly.
Prior to the introduction of Nervecentre screening, the number of patients administered antibiotics within one hour of a sepsis diagnosis was 29%. In May 2017, that figured had grown to 93% – and has continued to perform in excess of 90% in the months that have followed. Paul Latimer – Lead Nurse at County Durham and Darlington says :
The mobile platform is helping us support our staff with tools to recognise – and respond to – a potentially lifethreatening condition. And it’s allowing us to provide the assurance that every patient that comes into our care will be screened for sepsis – and treated promptly and appropriately.”
Automated, continuous cross-referencing of patient vital signs, lab results and clinical notes identifies potential sepsis, AKI or other conditions as soon as results are available – eliminating the delay and errors associated with manual checking of results
Automated workflows initiate time-critical actions, advising the most appropriate clinician of action required to manage each action through to completion
Each workflow is fully configurable to the process, escalation and alert policies appropriate to your hospital
Full audit and reporting of screening and actions for each condition
Includes the latest NEWS2 scoring system issued by the Royal College of Physicians.